Head and Neck Cancer Treatment

At UChicago Medicine, our head and neck cancer team strives to provide effective treatment that gives the patient the best outcome, while preserving as much speech, voice and swallowing function as possible.
The earlier the cancer is diagnosed, the more likely the treatment will be successful. Matching the appropriate therapy to each patient is vitally important in all cancer care.
For head and neck cancer, treatment may involve a combination of surgery, radiation therapy and/or chemotherapy. Experts in surgery, medical oncology, radiation oncology, radiology and pathology meet regularly in a head and neck tumor board conference to carefully review cases and work together to develop the best care plan for each patient.
Head and neck cancer treatment options are determined by the stage of the cancer, the location of the tumor and other factors.
Treatments include:
UChicago Medicine physicians pioneered an innovative first-line combination chemotherapy and radiation therapy approach that effectively shrinks some head and neck tumors, reducing the need for surgery. Patients with any type of head and neck cancer may be candidates for this approach.
For many patients with head and neck cancer, surgery is the best option for a successful outcome. Our expert head and neck cancer surgeons work with radiation and medical oncologists to develop a tailored treatment plan.
No matter the type or stage of cancer, if surgery is required, our experts provide the most effective treatment to preserve as much breathing, eating, speech and swallowing function as possible.
Some procedures may be performed using minimally invasive techniques or robotic surgery, resulting in a quicker recovery and less pain and scarring than open procedures.
We perform the full range of minimally invasive and traditional surgical procedures to treat cancers of the head and neck, including:
Endoscopic surgery: A minimally invasive approach that uses thin instruments to remove tumors with pinpoint precision.
Transoral robotic surgery (TORS):Uses sophisticated robotic technology to remove hard-to-reach tumors through the mouth, rather than creating larger incisions in the neck or jaw. Learn more about transoral robotic surgery.
Transoral laser microsurgery (TLM): A minimally invasive treatment for cancer in the voice box. During TLM, the surgeon gets a magnified view of the tumor with a microscope, and then uses a laser to remove it with precision, limiting the damage to nearby healthy tissue. This procedure preserves tissue and structures critical to voice and swallowing function.
Our radiation oncologists use sophisticated methods to deliver precise treatments to tumors while sparing healthy tissue.
UChicago Medicine was one of the first hospitals in the nation to offer intensity modulated radiation therapy (IMRT) for head and neck cancer. With IMRT, the radiation beam is accurately shaped to follow the contours of the tumor and to avoid critical structures such as the salivary glands or the optic nerve.
Our team also uses image-guided radiation therapy (IGRT) to confirm the exact tumor position and make any needed adjustments before treatment begins. Experts at UChicago Medicine refined a 3-D imaging system for IGRT, resulting in improved treatment planning and quicker radiation therapy sessions for the patient.
In recent years, cases of head and neck cancer linked to the human papillomavirus (HPV) have increased dramatically. HPV is the most common sexually transmitted disease in the United States and is the cause of most cases of oropharynx cancer (cancer of the tonsils and base of the tongue). Risk factors and prognosis for HPV-associated tumors are different from other types of head and neck cancers.
Our team has extensive experience treating patients with HPV-positive head and neck cancer. And we are at the forefront of research into how HPV-associated cancers respond to treatments. Our goal is to tailor effective therapies to reduce side effects and improve overall quality of life. Examples of outstanding care include robotic surgery, making treatment less intense and therefore better tolerated, and using new approaches that harness the power of the immune system to fight HPV-associated cancer.
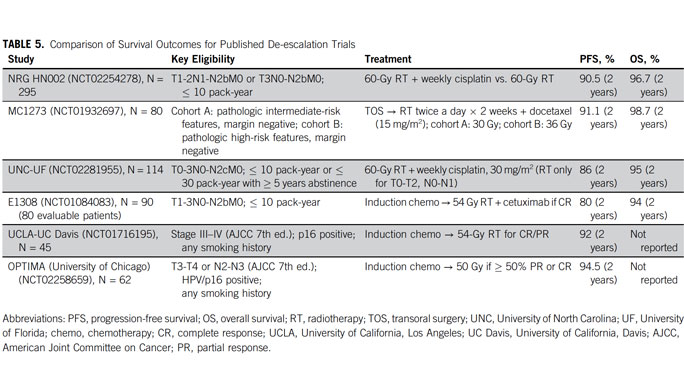
Read a Q&A about the role of HPV in head and neck cancer and how UChicago Medicine specialists are tailoring treatment for people with HPV-associated head and neck cancer. Our de-escalation approach resulted in the nation's leading survival rates: ~95% of patients were still alive after two years and patients treated with less radiation were less likely to need feeding tubes.
Immunotherapy — treatments that harness the power of the immune system to recognize and attack cancer cells — is an emerging treatment approach for head and neck cancer. Our physicians offer these treatments, in some cases as part of a clinical trial. As an example, a 2015 study here found that the anti-PD-1 immunotherapy pembrolizumab was effective in very advanced recurrent/metastatic head and neck cancers and roughly twice as effective as the best currently approved targeted therapy. In this study, immunotherapy was active across a wide range of patients, including HPV-associated and HPV-negative tumors.
Our head and neck cancer surgical team — which includes plastic and reconstructive surgeons who work with head and neck surgeons — are skilled at using organ-sparing and reconstructive techniques to maintain a patient’s physical appearance and function during and after treatment.
Patients with recurrent head and neck cancers often come to us after being told "nothing can be done." Our team believes that there is always something that can be done to support patients. Options may include surgery, radiation and/or experimental therapies. We work to provide pain relief, wound rehabilitation and hope for survival.
We are also leaders in re-irradiation — a second treatment, when necessary, of full-dose radiotherapy. This may involve a combination of radiation with chemotherapy and molecularly targeted agents.
Head & Neck Cancer: Q & A
Medical oncologist Alexander T. Pearson, MD, PhD, and nurse navigator Patricia Heinlen, BSN, RN, discuss head and neck cancer, including the HPV vaccine and how new treatment approaches are tailored to each patient's cancer type, making treatments more effective while reducing side effects.
Request an Appointment
We are currently experiencing a high volume of inquiries, leading to delayed response times. For faster assistance, please call 1-855-702-8222 to schedule your appointment.
If you have symptoms of an urgent nature, please call your doctor or go to the emergency room immediately.
For Referring Physicians
To refer a patient for head and neck cancer care, please call UCM Physician Connect at 1-800-824-2282.
* Indicates required field

Cancer Care Second Opinions
Request a second opinion from UChicago Medicine experts in head and neck cancer care.

Participate in a Clinical Trial
UChicago Medicine head & neck cancer experts are actively conducting clinical trials of new and promising treatments.

Helping You Cope With Cancer
Our Supportive Oncology program offers a range of services to support you and your family during your cancer treatment.
