Parathyroid Disease
Understanding Parathyroid Disease
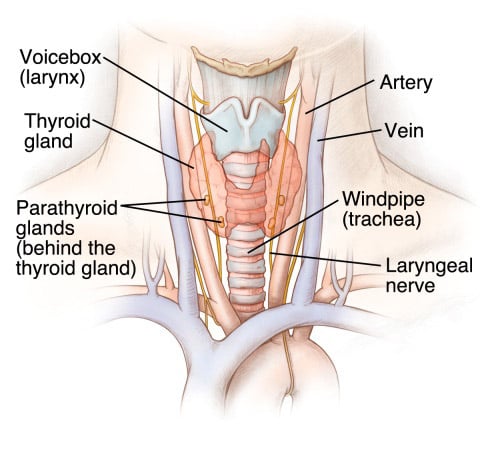
The parathyroid glands, which are located in your neck, constantly monitor and control the amount of calcium, phosphorus and magnesium circulating in your blood. When the level of these minerals rise or fall below normal, these four tiny glands adjust the amount of parathyroid hormone (PTH) they secrete. When more of this hormone is circulating, the bones release additional calcium into your blood. In contrast, when the parathyroid secretes less hormone, the bones give up less calcium. Vitamin D levels are also affected.
This vital balance can get disrupted when the parathyroid glands malfunction, due to a disease, injury or another cause. As a result, blood calcium levels get out of whack, causing one of two conditions:
- Hyperparathyroidism: When the parathyroid produces too much PTH, causing blood calcium to rise to unhealthy levels.
- Hypoparathyroidism: When the parathyroid is under-active, producing too little PTH and causing blood calcium levels to fall.
In addition to keeping bones strong, calcium plays a key role in other fundamental biological functions, including muscle contractions and communication between nerve cells. Thus, too much or too little calcium not only affects your bones but also your heart, digestive tract, kidneys, muscles and brain.
UChicago Medicine endocrinologists are among a select number of physicians in the region with strong experience in treating parathyroid disorders, including complex cases that may not be easy to diagnose or manage. Because we see a large number of patients with all types of parathyroid disease, we are able to pick up on indications in blood work and imaging scans that might be missed by less experienced physicians.
Our physicians are also world-renowned specialists in osteoporosis. Their combined knowledge and experience in bone and parathyroid diseases allows them to provide comprehensive care to patients whose bones are affected by parathyroid problems.
Treatment Options for Parathyroid Disease
There are two types of hyperparathyroidism, or over-active parathyroid:
- Primary hyperparathyroidism is when one or more of the four parathyroid glands secretes too much PTH, causing your calcium blood levels to rise. This may be associated with a risk of bone loss and kidney stones. It is often caused by a growth (typically noncancerous) on a gland or overactivity of one or more parathyroid glands. In rare cases, parathyroid cancer or genetic disorders (such as multiple endocrine neoplasia and familial isolated hyperparathyroidism) may cause overactivity.
- Secondary hyperparathyroidism develops when another disease or condition — such as kidney disease or a vitamin D deficiency — lowers the level of calcium in your body, causing the parathyroid to work overtime secreting more PTH in an attempt to balance calcium levels.
When patients have secondary hyperparathyroidism, our endocrinologists collaborate with other UChicago Medicine specialists to jointly address high calcium levels and the underlying medical problem. For instance, if kidney disease is causing hyperparathyroidism, then we work with nephrologists in our nationally recognized kidney disease program. Similarly, when secondary hyperparathyroidism is due to gastrointestinal problems causing poor nutrient absorption, we consult UChicago Medicine's gastroenterologists, who are among the best in the nation.
People with primary hyperparathyroidism who are experiencing symptoms typically have the dysfunctional parathyroid gland(s) surgically removed. Our endocrine surgeons use minimally invasive techniques for these procedures, whenever possible, which reduces scarring and pain.
Because primary and secondary hyperparathyroidism can look similar, our surgeons work very closely with our expert endocrinologists. Together, they review imaging scans and blood tests to ensure a patient has primary versus secondary hyperparathyroidism before undergoing an operation.
Removing a diseased or dysfunctional parathyroid gland(s) usually resolves blood calcium issues associated with primary hyperparathyroidism. Because people have four parathyroid glands, they can lose one or two without major side effects.
When parathyroid cancer is present, our endocrinologists collaborate with UChicago Medicine's highly experienced endocrine cancer team to develop a comprehensive treatment plan, which might include chemotherapy and radiation in addition to surgery.
Hypoparathyroidism, or under-active parathyroid, causes low calcium levels. The rare disorder may be caused by damage to the parathyroid (e.g., from a previous surgery), an autoimmune disorder, a genetic disorder or magnesium deficiency.
Hypoparathyroidism is typically treated with calcium and active vitamin D supplements, as well as a diet high in calcium. However, this conventional treatment approach does not always alleviate patients' symptoms.
Looking to further improve our patients' quality of life, our endocrinologists have collaborated with a team of national physician-scientists to study the potential of treating hypoparathyroidism with parathyroid hormone itself. As a result of such investigations, PTH therapy has been FDA approved for treatment of hypoparathyroidism and is available by prescription. However, initiating this novel therapy is rather complicated, and the expertise and experience of UChicago Medicine physicians is valuable in guiding patients through the use of this new therapy.
Request an Appointment
We are currently experiencing a high volume of inquiries, leading to delayed response times. For faster assistance, please call 1-888-824-0200 to schedule your appointment.
If you have symptoms of an urgent nature, please call your doctor or go to the emergency room immediately.
* Indicates required field



