Deep Brain Stimulation Surgery
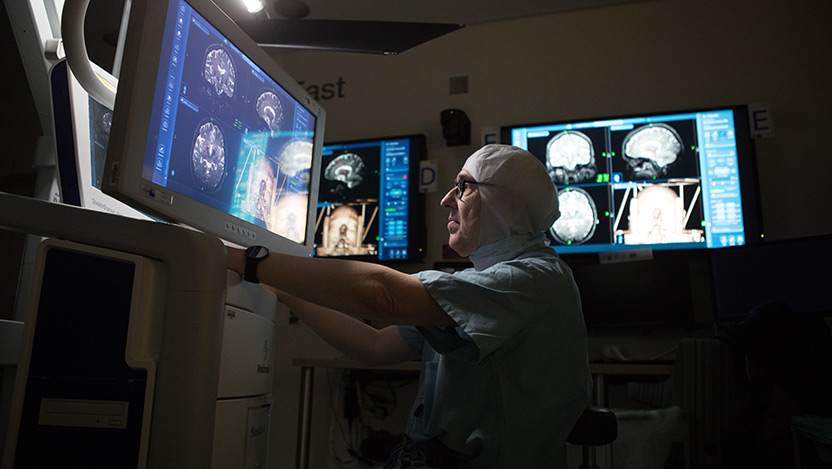
Deep Brain Stimulation Surgery
Our physicians are experts in deep brain stimulation (DBS) surgery. Almost all of our patients undergoing DBS surgery experience a significant reduction in the severity of symptoms. Additionally, our physicians actively research and develop techniques to enhance the effectiveness of DBS surgery.
DBS is a complex stereotactic procedure, meaning the neurosurgeon uses a 3D brain mapping system to access and treat precise areas in the brain that are otherwise difficult to reach. In stereotactic procedures, the neurosurgeon operates tiny, specialized surgical instruments through a very small hole in the skull while the patient is awake. This minimally invasive technique maximizes benefit and minimizes risk compared to traditional brain surgery.
DBS Surgery with Intraoperative CT
In addition to our team's unmatched expertise, we are the only hospital in the region with an intraoperative CT scanner in our operating room. This leading technology allows us to capture images of the brain during the procedure, which:
-
Enhances the accuracy and efficiency of device placement for the most effective results
-
Reduces the amount of time spent in surgery
-
Reduces the risk of post-operative infection
Percept PC DBS system
UChicago Medicine is the first hospital in the Chicagoland area to use the new Percept PC DBS system to treat patients with movement disorders and ranks as the most "Percept experienced" DBS program in all of Illinois.
The Percept PC DBS system not only stimulates the brain, but also takes recordings, allowing us to see how the brain responds to the stimulation. This system represents a new area of individualized treatment for our patients and should provide more symptom relief.
In DBS surgery, electrodes are placed precisely on the individual group of brain neurons responsible for movement in the affected body parts. With computer-assistance, pre-operative MRI scans and CT images taken during surgery are fused together to create a 3-D map of the patient's brain. Then, this map is overlaid with a digital brain atlas showing deep-seated structures in significant detail.
A tiny hole is carefully drilled in the patient's skull, starting the meticulous process of identifying the correct neurons inside the brain using hair-thin microelectrodes. These electrodes allow physicians to record activity so small that it can be traced to activity from one single brain cell. As the electrodes are placed, the neurosurgeon relies on the neurologist to elicit patient responses that confirm when the placements are correct. Patients must be conscious, but are kept very comfortable. Once each target in the brain is located, it is then stimulated to make sure the symptom is improved. If necessary, electrodes are moved millimeter by millimeter to gain the maximum benefits while minimizing side effects — all while patients are still in the operating room.
While electrodes are placed on one side of the brain, the team repeats the process on the other side. The entire surgery, including both sides of the brain, typically takes about six to eight hours. CT scans are taken during or at the end of the procedure to verify exact electrode locations and rule out any side effects — before the patient even leaves the operating room. Patients stay in the hospital overnight, and then return the following week to have the device's battery implanted under the collarbone in an outpatient procedure. After about four weeks, surgical healing is complete within the brain, and the neurologist activates and programs the DBS device to optimize the patient's symptom relief.
Deep brain stimulation (DBS) is FDA-approved for the treatment of patients with:
-
Essential tremor
-
Dystonia
Our physicians will carefully assess whether you are a candidate for DBS surgery. Eligibility must be determined on an individual basis. Specific criteria varies by condition, but may include factors such as severity of symptoms, progression of disease, response to medication, ability to tolerate surgery, psychiatric health, other present conditions, support system, and more.
Different types of deep brain stimulation (DBS) surgery target different parts of the brain. The best approach is determined by the patient’s symptoms, ability to tolerate the surgery, and risk of complications.
As leaders in DBS surgery, our team is skilled and equipped to perform:
Subthalamic DBS: One of the most effective treatments for patients with Parkinson’s disease in terms of the range of symptoms that can be alleviated and the ability to reduce the amount of medication patients need
Globus Pallidus DBS: A targeted approach for many patients with dystonias that may also be used as an alternative to subthalamic nucleus DBS in some patients with PD
Thalamic DBS: A preferred targeting method for patients with essential tremor that may also be able to treat other types of tremors
