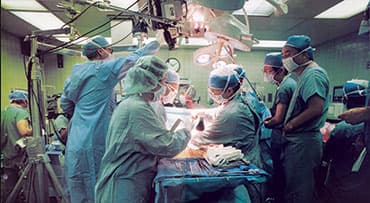
Heart Transplant Process
Heart Transplant Evaluation
For some patients with advanced heart failure, transplant may be the best treatment option. Our multidisciplinary transplant team completes in-depth medical, psychological and physiological evaluations of each patient to determine the individual's eligibility for transplantation.
Medical Examination
Transplant candidates undergo a medical screening process to ensure they are healthy enough for the procedure. Our heart transplant team looks for any indication of infection or disease that could be problematic post-surgery. The screening includes blood tests, pulmonary stress tests, diagnostic imaging and dental examinations.
Additional diagnostic testing may also be conducted to assess the health of the transplant candidate.
Psychosocial Evaluation
Candidates for heart transplant complete a psychosocial evaluation to determine if they have the motivation, family and emotional support, and psychological stability to handle the demands of heart transplant surgery and recuperation.
Physiological Assessment
Rehabilitation and physical activity are a large part of the recovery process after a heart transplant. By obtaining baseline information about our patient's current condition, we will have a better understanding of their physical limitations after surgery.
Waiting List
Once a patient is deemed eligible for a heart transplant, he/she is put on a waiting list managed by the United Network of Organ Sharing (UNOS). Patients are listed based on the severity of their condition. The length of time each candidate spends on the list can vary significantly.
Post-Transplant Care
After the procedure is complete, the heart transplant team monitors the patient's progress and manages all care during their hospital stay and throughout the recovery process. The first year after a heart transplant is especially crucial for combating rejection episodes, requiring everyone on the team — and the patient — to remain vigilant for any setbacks.
Frequently Asked Questions About Post-Operative Care
The length of the hospital stay depends on your progress, which your transplant team will monitor closely. Typically, patients are in the hospital for approximately two weeks following surgery.
Common signs of organ rejection include:
- Fatigue
- Fever
- Shortness of breath
- Swelling of ankles and feet
- Water retention/lack of urination
- Weakness
If you are experiencing any of these symptoms, contact your care team to evaluate your condition and decide what, if any, treatment is necessary.
Rejection occurs when the immune system recognizes the new organ as a foreign presence inside the body. The body's natural instinct is to neutralize, or attack, this object. Rejection is most common in the first six months after surgery.
In order to address this problem, patients take immunosuppressant medications to shut down the immune system's responses to the new heart. Because taking immunosuppressants can leave the body vulnerable to infection, patients are also be given antibiotics to counteract this threat. Adhering to the medication regimen is crucial for the success of your transplant.
Aside from medication, you will also have regular check-ups with your transplant team. You must maintain proper hygiene habits, including dental and dermatological hygiene, to prevent bacteria from interfering with your transplant success.
While the immediate few months after transplantation are an adjustment period, many transplant patients live full lives after surgery. Sustaining a healthy lifestyle is a permanent commitment. In order to promote long-term recovery, patients should maintain a healthy weight, participate in physical activity and remove/limit the use of harmful substances, such as tobacco, alcohol and caffeine. Taking these measures will reduce stress on your new heart and encourage optimal functionality.