Mesothelioma

Mesothelioma is rare. At UChicago Medicine, we treat it every day.
The University of Chicago Medicine Comprehensive Cancer Center has one of the largest mesothelioma programs in the world, staffed by some of the most experienced physicians in this rare disease.
Our multidisciplinary team cares for hundreds of mesothelioma patients every year, whereas oncologists and surgeons elsewhere may only see a few in the span of a career.
The breadth of our team’s expertise means we often set the standard of care for mesothelioma. We offer tailored treatment options, from advanced surgery and targeted chemotherapy to radiation therapy and clinical trials for promising new treatments.
Malignant mesothelioma is a rare cancer that is found in only a few thousand people each year in the entire U.S. This cancer can affect the abdominal area, chest cavity, or both. More specifically, it occurs in the mesothelium (also called pleura or peritoneum), a thin tissue lining covering internal organs, such as the lungs, heart, abdomen and testicles.
Mesothelioma is typically associated with exposure to asbestos. While asbestos is now rarely used in the U.S., it was historically a commonly used material. Asbestos can lead to mesothelioma many years later. Exposure in the 1970s and 80s can still affect people today.
Asbestos exposure doesn’t have to be direct to be dangerous. Secondhand exposure can also lead to mesothelioma. This can come in many forms, including, for example, living with a relative who worked in a factory, as a pipefitter, or as a mechanic on brake pads. Furthermore, some patients inherit changes in DNA that make them more likely to be sensitive to asbestos exposure.
There are causes of mesothelioma outside of asbestos exposure. Prolonged exposure to high radiation levels, particularly in specific medical or occupational settings, has also been suggested as a potential risk factor for mesothelioma.
Although mesothelioma is rare, the risk of developing the cancer increases with age. It’s more common in men than women, generally because more men worked in jobs with asbestos exposure.
Signs of mesothelioma are common in other illnesses as well, and it’s important to keep in mind that mesothelioma only affects about 3,000 people in the U.S. a year.
Some signs and symptoms of mesothelioma may include:
- Increased abdominal girth
- Significant weight loss
- Shortness of breath
- Pleural effusion (fluid in the chest)
- Changes in bowel movements
- Bowel obstruction
- Early satiety, which is feeling full soon after eating or from eating less than normal
- Abdominal or chest pain
- Decrease in appetite
- Persistent, dry cough
Mesothelioma is found in the chest and abdomen area – and in rare cases, in the testicles. Depending on its location in the body, mesothelioma can be referred to by different names. General mesothelioma describes mesothelioma that’s not confined to one specific area.
Pleural mesothelioma: Mesothelioma of the lining of the chest cavity. Pleural mesothelioma is often accompanied by fluid in the lungs and chest.
Peritoneal mesothelioma: Mesothelioma of the abdominal lining. It may cause fluid in the abdomen.
Pericardial mesothelioma: Mesothelioma of the lining of the sac which contains the heart. It typically causes fluid in the sac around the heart (pericardial effusion).
Mesothelioma of the tunica vaginalis testis: This is a rare form of mesothelioma in the lining of the testicles. It’s extremely rare and is less than one percent of cases of mesothelioma. Our team is experienced in this type of mesothelioma.
There are different subtypes of mesothelioma, with varying prognoses. Early detection is the best chance for improving treatment results.
Epithelioid: Named for the rectangular-shaped cells that resemble those found in epithelial tissues, like the skin or the lining of organs. Compared to the other subtypes, epithelioid mesothelioma tends have a slower growth rate. It typically responds more favorably to treatments like surgery, chemotherapy and radiation therapy.
Sarcomatoid: Characterized by the presence of spindle-shaped cells. It is often more aggressive and less responsive to treatment than the epithelioid subtype. Surgery is not a common treatment option.
Biphasic: A combination of both epithelioid and sarcomatoid cells within the tumor. Prognosis varies depending on the proportion of epithelioid and sarcomatoid cells and the tumor’s overall aggressiveness.
Early detection of mesothelioma can improve a patient’s prognosis. If your doctor suspects mesothelioma, they will generally order imaging tests such as an x-ray, MRI, PET scan or CT scan. Your doctor may also order an echocardiogram if they think there’s fluid around your heart.
Imaging can detect cancer and help to estimate the severity of mesothelioma. However, the final assessment of the type and staging of mesothelioma happens once your physicians gather tissue samples for lab analysis. Samples are usually collected during surgery, a bronchoscopy or needle aspiration.
After physicians identify the type and severity of mesothelioma, they will develop a personalized treatment plan that takes into account the stage of cancer, the biological characteristics of the tumor, as well as the patient's medical history and lifestyle. Physicians will recommend treatments that include surgery, chemotherapy, radiation therapy, or other targeted therapies.
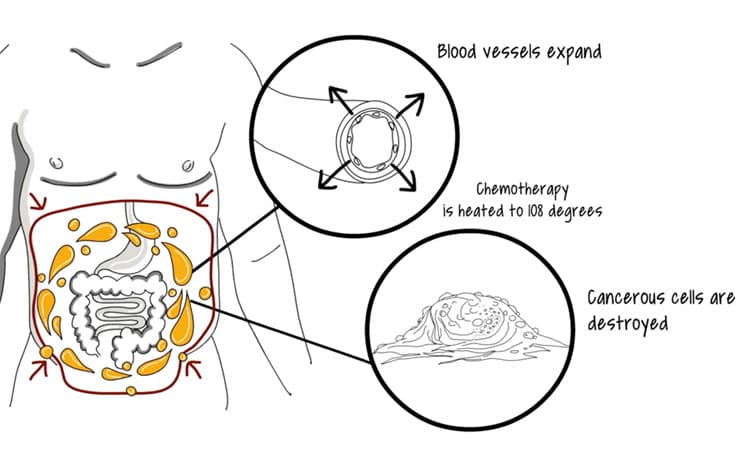
A key feature of the mesothelioma program at UChicago Medicine is HIPEC (hyperthermic intraperitoneal chemoperfusion). This targeted treatment attacks the cancer cells with a combination of surgery and heated chemotherapy directly into the abdomen.
Learn more about our full range of mesothelioma treatments.
A top goal for UChicago Medicine physicians-scientists is to identify and develop treatment regimens that improve the quality of life for people with mesothelioma.
In the past, most cancer science focused on common forms of the disease. However, as we learn more about how existing cancer treatments can precisely target mesothelioma cells in laboratory testing, more mesothelioma patients are being included in clinical cancer trials.
Patients receiving mesothelioma treatment at UChicago Medicine can access many national cancer trials. Your doctors can help you determine if a mesothelioma clinical trial is right for you.
What to expect from mesothelioma care at UChicago Medicine
You can expect personalized, expert care when you choose UChicago Medicine for mesothelioma care. A dedicated mesothelioma nurse navigator will focus on coordinating your care, and our team of mesothelioma experts meet weekly to discuss each patient's treatment.
Our patient-centered mesothelioma program includes a team of medical oncologists, thoracic surgeons, general surgeons, nurses, pathologists, imaging specialists and research scientists with deep understanding of the disease.
Our multidisciplinary clinical team and research scientists are internationally renowned for improving mesothelioma patient outcomes. Together, they’re dedicated to developing novel treatment protocols that extend and improve lives.
Meet our mesothelioma physician team.
Supportive Care
Our supportive care services are committed to helping you and your family during cancer treatment. This includes palliative care such as pain management, nutrition counseling, physical therapy and occupational therapy, social work services, and psychology and psychiatry services.
Our team of researchers has studied symptoms specific to mesothelioma and uses research-based insight to determine how to best support mesothelioma patients. The symptom management specialist works closely with the rest of our clinical team to ensure patients get the care they need.
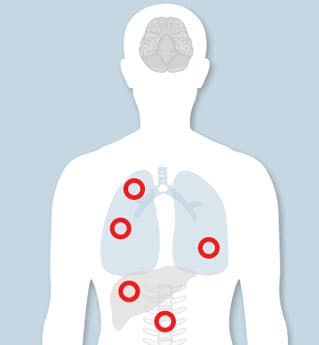
Treating Metastatic Cancer with Optimism and Hope
If you have been diagnosed with metastatic cancer, more therapies may be available to you than you think. Our cancer specialists are eager to help you understand all of your options.
Limited Metastatic Cancer Program
Cancer Care Second Opinions
Request a second opinion from UChicago Medicine experts in cancer care.

Participate in a Clinical Trial
Our physician-scientists are actively conducting clinical trials of new therapies for mesothelioma.
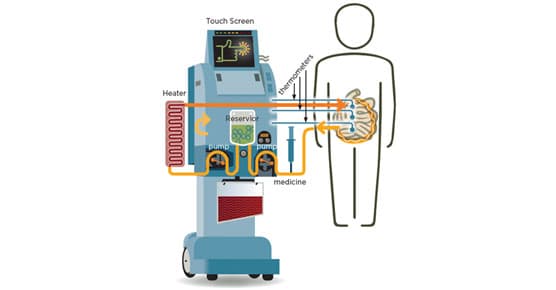
HIPEC: Targeted Heated Chemotherapy for Abdominal Cancers
HIPEC is targeted surgical technique that attacks abdominal cancer with fewer side effects than traditional chemotherapy.
Hyperthermic Intraperitoneal Chemotherapy (HIPEC)