'OR of the future' houses new tech to view the brain like never before
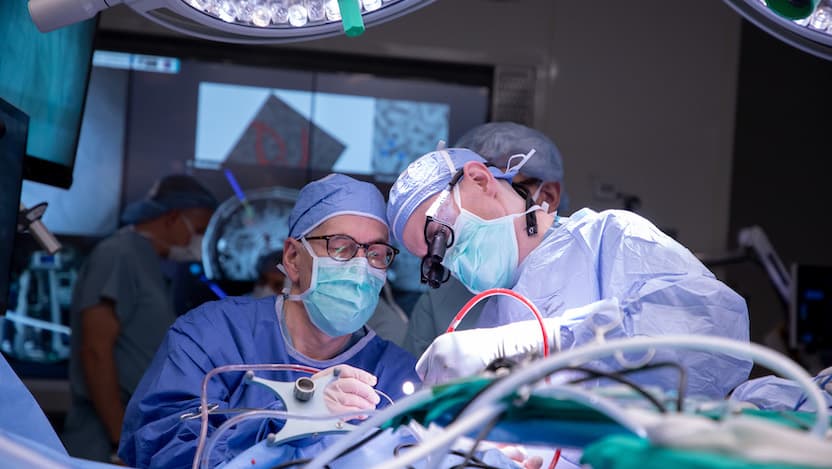
You may have heard stories of patients remaining awake and being asked to converse or even sing while receiving brain surgery. Although it may seem strange, this practice has long served as an effective way for brain surgeons to assess brain function mid-surgery to help ensure they don’t damage important tissue or neurons.
But leading neurosurgeons now have tools that far eclipse the precision of those “awake” brain surgeries.
At the University of Chicago Medicine, architects, builders, technicians and neurosurgery experts have collaborated to create a new kind of operating room designed to give physicians more information than ever to guide neurosurgical procedures.
"Our vibrant neurosurgery research program demanded real-time technology integration as the next logical step," said Peter Warnke, MD, Director of Stereotactic and Functional Neurosurgery at UChicago Medicine.
This “OR of the future,” as Warnke called it, opened in January 2023, and it features cutting-edge instruments and high-definition screens that allow brain surgeons to scan and view key areas of the brain throughout an operation.
Since then, UChicago Medicine neurosurgeons have used the technology for procedures as intricate and precise as electrode implantation and laser surgery that restored a patient’s senses and left them seizure-free.
Functional imaging mid-surgery
Warnke says the highlight of the technology integration is a new intraoperative MRI recently installed in the OR at UChicago Medical Center in Hyde Park.
Now, doctors can run functional MRI (fMRI) scans mid-surgery to see not only how the brain is arranged but also how it’s working in real time. This can include looking at the brain’s response to surgical interventions like electrical stimulation, performing metabolic imaging to see how different brain cells produce and use energy, and tracking physiological responses.
The installation required significant planning: MRI technology requires copper shielding to be built into the room’s walls to prevent outside radio frequencies from distorting the imaging and to shield the outside world against the powerful magnetic field generated by the magnet.
In addition to the intraoperative MRI technology, UChicago Medicine has also added two complementary mobile CT scanners, including a ultrafast, 64-slice helical scanner that can be wheeled around for use in multiple ORs.
As part of this 3D imaging setup, the Department of Neurosurgery also recently acquired new neurosurgical robots — the Autoguide and ROSA systems — to make all surgeries as precise and safe as possible.
“We can combine intraoperative MRI scans and functional imaging with intraoperative CT scans and robotics during surgery, allowing true hybrid surgeries that give us the best advantages of all these technologies,” Warnke said.
'A major paradigm shift'
UChicago Medicine staff can use the OR’s high-definition wall screens to view output from the MRI, CT scans and all surgical plans, including robotic trajectories and relevant images from a patient’s medical record. The ability to refer to these images throughout surgery can help surgeons individualize their surgical approach down to the millimeter.
“In each patient, we’re able to evaluate the brain circuitry and target those circuits precisely and individually,” Warnke said.
They can also look at the connections between different areas of the brain, which is essential for complex procedures like pediatric epilepsy surgery and treating deep-seated tumors.
“We have moved from simplified removal of brain tissue to sophisticated disconnections and modulation of seizure onset zones,” Warnke said. “With precise imaging, we can use minimally invasive tools like interstitial lasers and responsive closed-loop stimulation systems to reduce morbidity significantly. It’s a major paradigm shift in neurology.”
Each surgical step can include a new scan that allows experts to update the surgical plan and confirm accuracy. And when surgeons are removing or destroying a tumor, they can perform a scan to ensure the treatment is as complete as possible before closing incisions.
Warnke said the new OR setup also will enhance the education of trainees at the academic medical center.
“It’s invaluable for trainees to see the effect of a surgery visually while it is being performed,” he said.
Enabling tomorrow’s neuroscience
For years, UChicago Medicine has been a leader in brain-computer interface research related to motor control and sensation. Warnke has performed surgeries that re-created a sense of touch and motor control via prosthetic hands for paralyzed patients, most recently in one of the new ORs.
“The impact of intraoperative imaging on our brain-machine program in particular is huge,” Warnke said. “We can now look at brain function as we are placing an electrode or laser fiber, thus guiding it more precisely than ever before.”
Immediately after an implant is placed, neuroscientists can use the various imaging technologies to test the implant’s function before concluding the surgery. This allows them to collect important data for research analysis and also make sure the implant is working properly, minimizing the need for follow-up surgeries to tweak its placement.
In October 2023, the UChicago research group received a $3.4 million R01 grant from the National Institutes of Health to further propel their research into developing more sophisticated brain-computer interfaces. Specifically, the researchers aim to develop brain-computer decoders that emulate the seamless coordination of arm and hand movements — and to test these advanced decoders within a virtual reality environment that simulates daily activities.
Warnke emphasizes that he is just one member of the university’s “vibrant neurosurgery research program.”
For example, colleagues at the Grossman Center for Quantitative Biology and Human Behavior are bringing unparalleled computational techniques to vast neuroscience datasets, while others are investigating ways to improve treatments for epilepsy, vascular malformations and brain tumors with less invasive diagnostic techniques and more effective surgeries —efforts that will receive a boost from the new OR’s capabilities.
“It’s all part of a wider realm of innovative neuroscience that is bringing new technology and exciting research with immediate benefit for the patient to the OR,” Warnke said.

Peter Warnke, MD
Internationally renowned neurosurgeon Peter Warnke, MD, has performed more than 5,000 stereotactic surgeries and more than 2,000 brain tumor surgeries. Dr. Warnke provides neurosurgical care for the treatment of adults and children with movement disorders, epilepsy and brain tumors.
Learn more about Dr. Warnke
Our Level 4 Pediatric Epilepsy Center
At Comer Children's Hospital, we offer the skill, experience and technology to definitively diagnose childhood epilepsy. Our team of experts provides the highest level of medical and surgical care for complex epilepsy in children of all ages.
Childhood Epilepsy & Seizures