Balloon pulmonary angioplasty relieves symptoms of CTEPH

James Jackson, 74, first learned he had blood clots in his lungs more than 30 years ago.
“I became breathless if I moved too quickly or lifted something,” said Jackson, who at the time worked for a telecommunications company in Ft. Wayne, Indiana. “One day I blacked out while on the job.”
Jackson was treated with blood thinners to keep the clots from getting larger and to prevent new ones from forming. But over time, the clots caused scarring, which narrowed the blood vessels in his lungs. This brought on pulmonary hypertension – high blood pressure in the arteries that go from the heart to the lungs. This condition forces the heart to work harder to pump blood through the lungs.
When his symptoms worsened over the past few years, Jackson’s cardiologist in Indiana recommended he see the pulmonary hypertension experts at the University of Chicago Medicine.
James was having difficulty breathing even just around the house. His heart could not keep up with delivering enough blood to the brain and the rest of his body.
Our pulmonology team diagnosed Jackson with chronic thromboembolic pulmonary hypertension (CTEPH) — scarring and chronic blockages of arteries in the lungs. Medications were no longer effective in restoring blood flow to his lungs. Without more aggressive treatment, the condition would lead to congestive heart failure and death.
A surgery called pulmonary thromboendarterectomy (PTE) can cure patients with CTEPH. The extensive operation removes the blood clots and scar tissue from the lung’s major blood vessels. At the time, UChicago Medicine had not yet started offering PTE, and the pulmonology team recommended Jackson go to UC San Diego Health, the hospital that pioneered the procedure.
Jackson flew to California and had PTE surgery the day before Thanksgiving in 2019. But residual clots in the tiny vessels of his lungs could not be reached and removed. Unfortunately, the procedure brought only minimal relief. Back home, Jackson continued having shortness of breath and had to be hospitalized at UChicago Medicine on Christmas Eve.
Jackson’s family began to lose hope. “We thought if the surgery didn’t work, nothing would,” said his daughter Sharon Hollis, who lives next door to her parents.
But interventional cardiologist Jonathan Paul, MD, offered another solution. Balloon pulmonary angioplasty (BPA), a new minimally invasive procedure, could restore blood flow in his lungs.
BPA involves the insertion of a small catheter in a vein in the groin, which is then threaded to the affected arteries in the lung. A small, deflated balloon is guided through the blood vessels to the blockage, where the balloon is inflated, breaking up scar tissue and pressing old clots against the artery walls. Each BPA procedure takes about two hours, with most patients needing between three and six sessions, depending on the extent of their disease.
Because BPA doesn’t require general anesthesia, Jackson was awake during each of his treatments in UChicago Medicine’s cardiac catheterization lab.
“He watched each angioplasty on our cath lab screens and asked questions as we went along,” Paul recalled. “He tolerated the procedures very well and had no pain.” By the time Jackson completed four sessions, the pressure in his lungs had come down by more than 50%.
Today, Jackson reports feeling better than he has in years. Hollis says her father seems like a “totally different person.”
“He can walk a long distance to the mailbox and has started riding a bicycle,” she said. Jackson is once again enjoying time in his pole barn, where he tinkers with small engine repair and usually has two or three projects going at once.
The UChicago Medicine Comprehensive Venous Thrombosis and Pulmonary Embolism Program now offers the full range of treatments — medication management, PTE surgery and BPA for CTEPH. Each patient is evaluated by a multidisciplinary team including radiologists, hematologists, pulmonologists, cardiac surgeons and interventional cardiologists to determine the best course of care.
“It’s really gratifying to see James do so well,” Paul said. “We want to reach out to more CTEPH patients like him and let them know that innovative new treatments are available. It’s very possible to give them back a good quality of life.”

Jonathan Paul, MD
An interventional cardiologist, Jonathan D. Paul, MD, uses minimally invasive, catheter-based techniques to diagnose and treat cardiovascular diseases. In particular, he provides care for patients with coronary artery disease, peripheral vascular disease, aortic disease and structural heart disease.
Learn more about Dr. Paul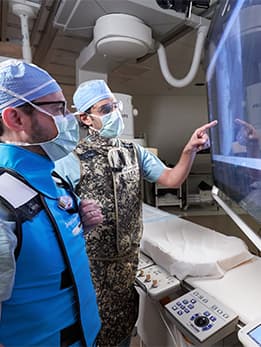
Comprehensive Venous Thrombosis and Pulmonary Embolism Program
Blood clots can be dangerous, and even fatal, if you do not receive treatment in a timely manner. The University of Chicago Medicine, our multidisciplinary venous thrombosis and pulmonary embolism team works closely together to quickly identify, screen, diagnose and treat these conditions.
Learn more about our services.