Lung transplant patient with COVID-19 recovers following plasma clinical trial
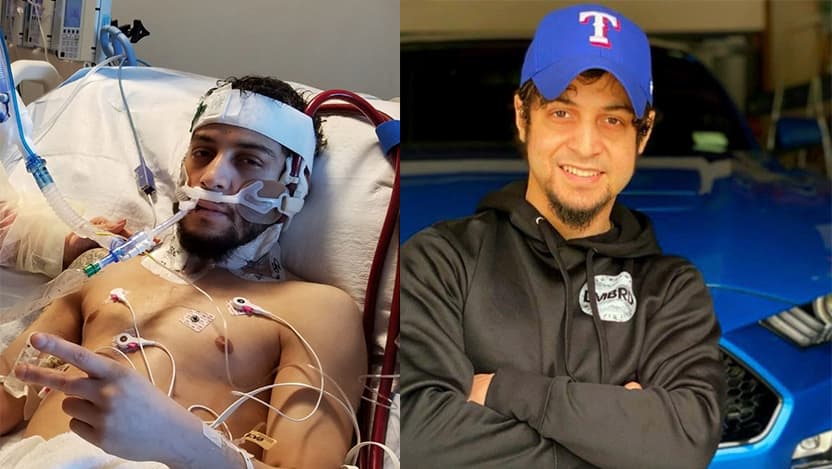
A year after his successful lung transplant, Edgardo Diaz, 30, found himself back in the hospital with COVID-19. Feverish and with failing kidneys, his condition quickly became critical.
Running out of time and options, Diaz’s doctors at the University of Chicago Medicine invited him to participate in one of the hospital’s COVID-19 clinical trials where he’d receive convalescent plasma – plasma rich in virus-fighting antibodies, taken from the blood of COVID-19 survivors.
Diaz, an Oak Forest resident, is believed to be the first lung transplant patient in the world to receive convalescent plasma for COVID-19. He might even be the first person worldwide with any type of transplant to receive the COVID-19-fighting plasma.
Within hours after receiving the convalescent plasma on April 25, Diaz’s 104-degree fever started going down. Days later, his breathing and kidney function improved. Nine days after receiving the plasma, Diaz tested negative for COVID-19. He was released from the hospital May 1, and continues to test negative for the virus.
Now that he’s home, Diaz said he feels “even better than I did before I had COVID-19.” He’s been able to resume his workouts, and has returned to his job.
Diaz stayed in close contact with his transplant team throughout the whole process. They knew his lung transplant disqualified him from most COVID-19 trials. But because he had severe and possibly life-threatening COVID-19, he met the FDA criteria for UChicago Medicine’s plasma trial, said Maria Lucia Madariaga, MD, who heads up the trial and was one of Diaz’s lung transplant surgeons.
Despite Diaz having a suppressed immune system from his lung transplant, his doctors decided that the convalescent plasma would be a low risk treatment for him – just as low risk as it is non-transplant patients.
“It’s a pretty safe therapy,” Madariaga said, adding that early reports she’s seen nationwide about giving convalescent plasma to COVID-19 patients has shown very few side effects. “We have given it to high-risk, immunocompromised patients, and it still seems safe.”
Unlike most hospitals in the U.S., which buy blood from a private company, UChicago Medicine has its own blood bank with more than 100 plasma donations from former COVID-19 patients, to aid the clinical trial.
“For a disease like COVID-19, with so many unknowns, it’s great that we’re able to offer this and other clinical trials,” Bag said.
Bag doesn’t believe this convalescent plasma treatment will work for everyone, although it seems like a promising treatment for some patients.
“I don’t think we have enough evidence,” Bag said. “We need to more vigorously study the treatment. You get great results in some patients and not in others. Edgardo did remarkably well.”
Researchers are still studying COVID-19, but it appears similar to a viral pneumonia in the lungs. It causes an overactive immune response, attacking the lungs and kidneys, and causing infection and inflammation in the body. If the immune system doesn’t or can’t respond to the virus, it can be deadly, Bag said.
When someone is infected with COVID-19, the body’s immune system produces proteins called antibodies that, in most cases, will seek out and neutralize the virus. They provide the immune system extra resources to fight off the infection. Those antibodies then stay in the blood and provide immunity. That’s why the plasma from COVID-19 survivors is valuable to those who are very ill.
COVID-19 isn’t disproportionately infecting lung transplant patients – they are equally susceptible as the general population, Bag said. They may be even more protected, because they’re very cognizant of infections, and have practiced mask-wearing, social distancing and hand washing following their transplants, long before COVID-19 came along.
As for Diaz, he’s continuing to wear a mask, wash his hands often, and take extra precautions not to catch germs.
“Everybody’s different, but the plasma did pretty well with me and I think it’ll do well with someone with new organs, also,” Diaz said. “I beat coronavirus! At this point, nothing’s going to stop me.”
Anyone over the age of 18, who had a documented case of COVID-19 and has been symptom-free and healthy for more than 14 days, is encouraged to donate plasma at UChicago Medicine.
Lung Transplantation at UChicago Medicine
Whether you have a straightforward condition or a very complex case, our lung transplant specialists have the expertise to help you. We treat a variety of lung conditions, including cystic fibrosis, pulmonary hypertension, Alpha-1 antitrypsin deficiency and pulmonary fibrosis.
Read more about our lung transplant program
Maria Lucia Madariaga, MD
Maria Lucia Madariaga, MD, is a highly skilled thoracic surgeon who specializes in a wide range of lung conditions, including airway disorders, benign and cancerous esophageal disease, and metastatic tumors.
Learn more about Dr. Madariaga