Pulmonologist helps create new robotic device to detect lung cancer earlier than ever before

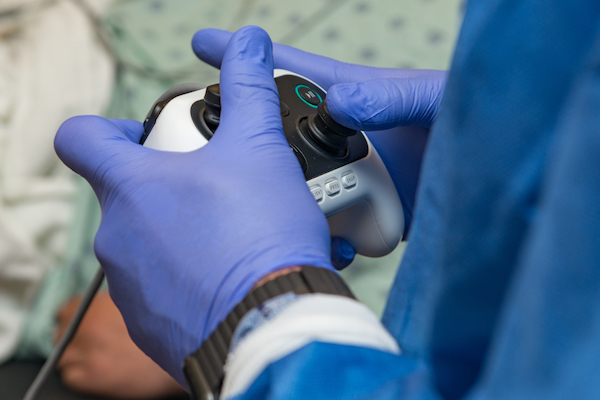
Facing a glowing screen and with a small, thumb-controlled device in hand, pulmonologist and advanced bronchoscopist D. Kyle Hogarth, MD, FCCP, looks like he could be playing a video game. Instead, he’s inside a room at the University of Chicago Medicine, guiding a new robotic device deeper into the lungs than most physicians have ever gone before.
Hogarth is an expert in advanced bronchoscopy, a minimally invasive procedure that lets physicians see inside a person’s airways with the help of a small camera (or scope) attached to a long tube that's inserted through the mouth. For years, he'd been frustrated by the existing technology’s limitations: a single scope and its rigid casing can only navigate so far into the vast landscape of the lungs. Even more frustrating? Much of the detailed work to position the device inside the intricate and delicate spaces had to be manually done by the doctor.
Several years ago, Hogarth was approached by a medical device company in need of a physician consultant to help them realize a bold vision: the creation of a robotic device that would attempt to remedy scoping's existing limitations and get physicians farther into the body with greater precision and accuracy. Hogarth jumped at the chance.
“They pitched the vision, and I knew nothing like it existed,” he said. “As soon as I heard their goals, I said, ‘I know what you’re trying to accomplish, and that’s amazing. I’m in.’”
Hogarth signed on as the chief pulmonology consultant for Auris Health, a Redwood, Calif.-based device company, to help create the Monarch Platform. On March 26, 2018, the U.S. Food and Drug Administration cleared the technology for robotic bronchoscopy. (The company hopes to eventually get approval for other uses, as well.) Three months later, UChicago Medicine became the second hospital in the nation -- and the first in the Midwest -- to begin using the novel platform.
In his role as a consultant, Hogarth took the earliest iterations of the machine for test drives in models and cadavers and helped keep the developers on task to create something that could truly revolutionize patient care, especially for people with lung cancer.
“Having someone like me there reminded them of what the field of pulmonology needs,” he said. “The engineers are ridiculously smart, but they needed to be pushed in the direction our patients need them to go.”
While Hogarth cares for people with everything from respiratory distress to severe asthma, the majority of his patients are awaiting confirmation of their worst fears – a lung cancer diagnosis. Lung cancer is a growing problem in the U.S. and is the leading cancer killer of both men and women. Most lung cancer diagnoses come at a late-stage, resulting in five-year survival rates that are under 20 percent. Physicians and patients desperately need diagnostic advances to help spot and treat cancer earlier, Hogarth said, which gives them the best chance of catching the disease before it becomes deadly.
Since I’ve begun using the device, I’ve been able to see patients I would have had to turn down previously ... It’s a brand new opportunity for patients, and that alone is exciting.
When patients who suffer from chronic breathing problems see a UChicago Medicine pulmonologist, such as Hogarth, they have their lungs viewed with a tiny camera at the end of a scope. The physician then samples problematic tissue on the spot, and a pathologist in the room analyzes the retrieved sample for any abnormalities.
When patients wake up from sedation, Hogarth and his team walk them through the results of the evaluation and map out a treatment plan that might include surgery to remove the cancer.
Prior to having the Monarch Platform, Hogarth was more limited in the types of patients he could evaluate and the tissue he could reach. He now has 360-degree visualization in the airways, and a nested scope design allows one scope to stay planted while the second ventures on to the exact spot being targeted, making hard-to-navigate s-curves in the lungs no longer insurmountable.
“Since I’ve begun using the device, I’ve been able to see patients I would have had to turn down previously,” he said. “I would have known I couldn’t get to their issue. That’s huge. It’s a brand new opportunity for patients, and that alone is exciting.”
Currently, Hogarth uses the machine largely as a bridge to the far-reaches of the lung for more accurate diagnoses. As exciting as this new technology is, he believes it is just the beginning. Hogarth envisions a time in the near future where pulmonologists can spot and diagnose cancerous lung tissue and then immediately kill it through a device that delivers targeted microwaves.
“Now I have a tool that gets me to a spot deep in the lung,” he said. “From there, the sky’s the limit.”

D. Kyle Hogarth, MD
D. Kyle Hogarth, MD, is an expert in pulmonary diseases — including lung cancer and alpha-1 antitrypsin (AAT) deficiency. He is an expert in the minimally invasive diagnosis, management and staging of lung cancer through bronchoscopy. He is a leader in advanced bronchoscopy using electromagnetic navigation systems that employ 3D imaging technology to detect and biopsy lung nodules and masses.
Read Dr. Hogarth's physician profile.
Lung Cancer Care
At UChicago Medicine, we offer a wide range of lung cancer care options, including minimally invasive surgery and innovative targeted therapies, as well as clinical trials of promising treatments not widely available.
Learn more about our lung cancer care.