Leakage, Bleeding, Irritation and Other Common Ostomy Pouching System Issues
Leakage
A pouching system should stay sealed to your skin for a predictable amount of time, and there should be no leakage under the adhesive seal between the time you place the pouching system on to when you take it off.
There can be many reasons that the pouching system may leak. Below are some common causes and suggested solutions.
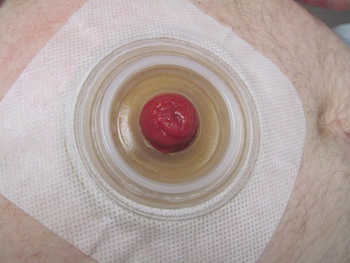
- The size in the skin barrier should match the size of the stoma. If the opening in the skin barrier is too large, the stool can make contact with the skin and loosen the adhesive seal.
- The shape of the skin barrier does not match the shape of the peristomal skin (the skin around the stoma). If the skin around the stoma does not remain flat when sitting or standing the skin barrier may pucker and allow stool to undermine the seal. If this is the case the use of a convex pouching system may help keep the peristomal skin flat. Skin barriers are available in a flat or convex shape. One way to determine which shape is best for you is to examine the peristomal skin in a sitting and standing position. If there are creases in any position consider the use of a convex pouching system.
- If the stoma does not protrude above the skin, the stool may get under the pouch seal and cause leakage. A convex pouching system can provide some pressure around the stoma to force output to get into the pouch and not under the skin barrier seal. If the pouching system is worn for a prolonged period of time, the skin barrier/adhesive can erode or wear away and this can cause leakage. If this happens, consider decreasing wear-time by one or two days.
If you are unable to determine why your pouching system is leaking, make an appointment with the ostomy nurses in the stoma clinic for an evaluation.
Skin Problems
If the skin around the stoma does not appear to be similar to the skin on rest of your abdomen, it is likely that you have a skin issue that needs to be addressed. The skin barrier should protect your skin. If the skin is irritated (red, moist, or sore to the touch), the pouch seal can fail and leakage.
The first step in treating red skin is to correct the underlying problem issue.
Be sure that the fit of the skin barrier is adequate (see above), that you are using the correct size and shape of skin barrier (see above), and that you are wearing the pouching system for a reasonable amount of time.
A less common cause for red irritated skin around the stoma is a reaction to the products in the pouching system.
In this case, the redness is located in the area where the offending product is located. A new product should be considered.
If the cause for the irritation cannot be determined, make an appointment in the stoma clinic. Our ostomy nurses will work with you to help identify and correct the cause of the problem.
Once the reason for the skin irritation is determined and the cause corrected consider treating the irritated skin as follows: after gently cleansing the area with warm water, and drying the area, sprinkle the irritated skin with skin barrier powder, rub gently into the skin and brush off the excess. Apply the new pouching system. The skin barrier powder can dry the skin to provide a dry surface to adhere the pouching system.
Use this online tool to help you assess your peristomal skin
Pictures of Common Stoma Skin Issues
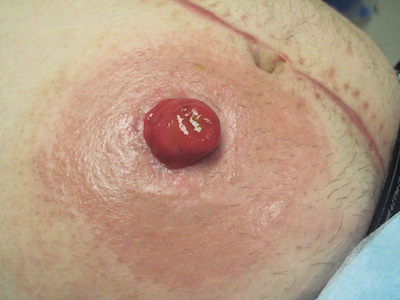
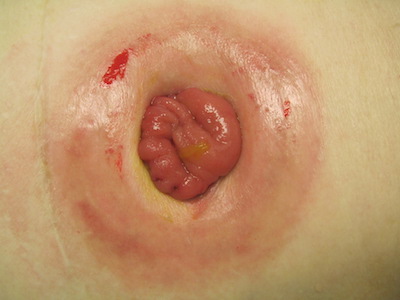
Denuded skin refers to skin irritation caused by exposure to urine, feces or body fluids. This image shows denuded skin of a patient with a loop ileostomy.
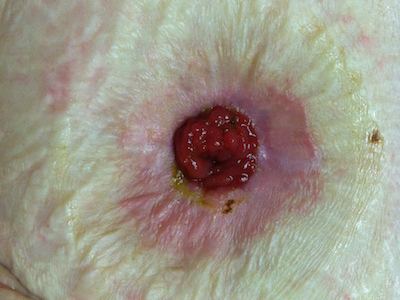
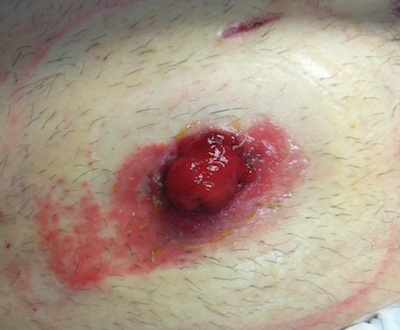
Bleeding
What should you do if you notice blood in or around your stoma?
First, examine your stoma and determine where blood is coming from. Then gently press the spot with a clean, dry pad. This usually stops the bleeding.
If minor bleeding continues for more than a few minutes, or if you notice blood in your stool, please contact your ostomy nurse for guidance.
In rare cases when bleeding is heavy, this could be a sign of a larger problem. Go to the emergency room for immediate treatment.
Complications/Medical Emergencies
Contact your ostomy nurse or other health care provider immediately if you experience:
- Bowel obstruction (no stoma output for greater than 5 hours accompanied by pain, bloating, nausea and/or vomiting).
- Dehydration (inability to maintain a good fluid balance, feeling lightheaded and dizzy, always thirsty, high liquid stoma output).
If you are unable to contact your ostomy nurse or health care provider, go to the local ER.
Additional Resources
Find an ostomy support group near you on the UOAA site.

Nationally Ranked in Gastroenterology and GI Surgery
According to U.S. News & World Report's 2024-25 Rankings.
Learn more about U.S. News Best HospitalsRequest an Appointment
We are currently experiencing a high volume of inquiries, leading to delayed response times. For faster assistance, please call 1-888-824-0200 to schedule your appointment.
If you have symptoms of an urgent nature, please call your doctor or go to the emergency room immediately.
* Indicates required field
