What you should know about sleep apnea
Sleep is one of the most fundamental processes for our health, but sometimes our bodies get in their own way. Inspire therapy, which involves hypoglossal nerve stimulation. The hypoglossal nerve controls the back of the tongue.
In this expert Q&A, LoSavio offers insights into what patients, family and friends can learn about the condition and describes the ever-broadening array of treatments and management strategies that can improve quality of life.
What is sleep apnea?
Sleep apnea involves pauses in breathing when you're sleeping at night. There are two types of sleep apnea. The more common type is obstructive sleep apnea, in which people stop breathing due to an anatomical obstruction in the throat. The less common type is central sleep apnea, in which the body fails to initiate a breath. That typically happens in patients who have issues with their central nervous system or cardiac problems.
What are some of the symptoms or warning signs of sleep apnea?
Most people’s first step towards a sleep apnea diagnosis is having a family member or friend let them know that they have abnormal breathing patterns and snoring at night. Otherwise, people just find themselves noticing daytime tiredness despite getting a full night's sleep.
In today's busy world, we often assume that being tired all the time is normal. This can be especially true for people in middle age with busy families. It’s true that life is hectic, but a lot of times that fatigue can be a sign of an underlying medical issue.
What can be the consequences of untreated sleep apnea?
Sleep apnea affects people in four ways:
- Quality of life: Patients often feel tired and may start to notice poor performance at work.
- Interpersonal relationships: Sleep apnea can affect not just the patient, but also the people around them. Loud snoring, for example, can be very disturbing. I have lots of patients who talk about having to sleep in separate bedrooms, which can have a significant effect on relationships.
- Health: Patients with moderate-to-severe sleep apnea have an increased risk of adverse cardiovascular events and higher mortality rates.
- Safety: Patients with sleep apnea are at higher risk for accidents during everyday tasks like driving. It can be a particular concern for people with certain occupations, such as those operating heavy machinery.
What management strategies or treatments are available for sleep apnea?
Once patients get a diagnosis, there are some management strategies they can implement by themselves to optimize their sleep health:
- Change sleeping position. Many people do better sleeping on their side rather than their back. In addition, sleeping with the head somewhat elevated can help reduce sleep apnea events.
- Decrease smoking and alcohol intake. When people drink or smoke, they snore more because those substances relax the muscles in the back of the throat.
- Optimize nutritional and physiologic health. Obesity is linked strongly with sleep apnea, although it’s by no means a one-to-one relationship.
Medical treatments involve some type of device or procedure:
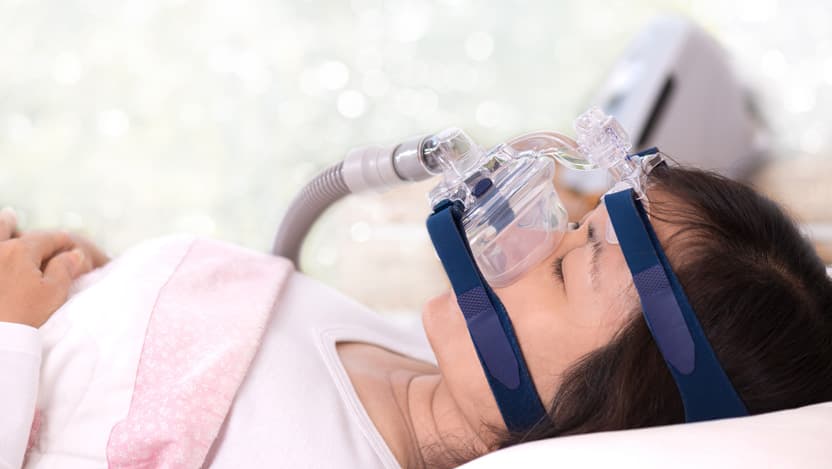
- CPAP (continuous positive airway pressure) machine. Patients can be fitted for a mask connected to a machine that provides a steady flow of air, which creates pressure to keep their airway open and prevent it from collapsing. This is generally the first-line treatment.
- Dental or oral appliances. For some people, devices inserted into the mouth before sleep can hold the airway open by pulling the jaw and tongue forward.
- Surgery. A surgeon can implant a device or modify the anatomy of the upper airway to allow it to stay open.
How are you working as a UChicago Medicine physician to treat sleep apnea?
First of all, I work to identify why patients have sleep apnea so we can have more advanced diagnostic tools to choose the right treatment for each person. For all patients being considered for a surgical sleep apnea intervention, I do a 10–15 minute procedure called sleep endoscopy, where we look at their throat during a brief period of sedation to identify all the different areas of obstruction that aren’t evident when they’re awake. We also measure the opening pressures of the throat to determine how easily collapsible their throat is, which can give us a sense of how well they'll respond to a procedure. I’ve done over 1,000 sleep endoscopies, so I’m able to predict what will work for each individual.
On the therapeutic side, I specialize in surgically implanting a hypoglossal nerve stimulation device, which has been a paradigm shift in how we treat sleep apnea since it received FDA approval in 2014. It’s a low-risk yet complicated surgery, but I do it multiple times every week so patients can be confident in the outcome. We implant a neurostimulator on the chest wall and attach a wire lead to the hypoglossal nerve, which controls the back of the tongue. Patients use a remote control to turn the device on before bed, and it stimulates the muscles to prevent the throat from collapsing every time they take a breath at night.
Are there any barriers that hinder patients from accessing hypoglossal nerve stimulation technology?
Lack of awareness is what most frequently hinders access. Even if people see advertisements for the device, they often don't fully understand what it is. Fortunately, physicians are beginning to learn more about what it is and who it can help.
One barrier that was recently lowered is eligibility. The FDA recently opened the indications to a broader population in summer 2023, meaning more people can be candidates for this treatment. There used to be significant limitations related to weight and sleep apnea severity index. Now the eligibility requirements have now been expanded dramatically.
How is sleep apnea treatment continuing to evolve?
I believe the future of the field is combining multiple therapies. Some sleep apnea medications are currently in clinical trials. It’s unlikely that those medications will be fully effective on their own, but as we’ve learned with cancer therapies, it’s possible to combine different treatments to give patients the best outcome. I can envision patients going through a complicated diagnostic algorithm that can predict, ‘This patient is likely to benefit from this surgery with this medication and a small device they can wear at night.’ I also expect to see other technologies and treatments emerge in the coming years. New, groundbreaking technologies tend to open up innovation in other areas.
What is the focus of your sleep apnea research to improve patient care in the future?
I am studying the effect of sleep apnea on people's overall metabolic health. I think patients who are metabolically unhealthy may be more predisposed to sleep apnea, which in turn can cause people to have cardiovascular health problems or other issues — almost a circular effect. So we’re interested in studying not just how treatments affect numbers on a test report, but ultimately the real long-term effect. How can we help patients live longer? How can we improve their blood sugar and blood pressure — all these really important things their doctors monitor? These are the questions we want to answer.
What is most important for people to keep in mind?
Sleep is one of the core health factors tied to our wellness and longevity. So if you feel like you're not sleeping well, you shouldn't just accept that as a byproduct of our busy lives; you should seek out solutions. If you have sleep apnea and treatments haven’t made a significant difference so far, you should know that there are probably other options out there.
Know that your healthcare providers will take it pretty far in terms of trying to find a good solution for you. I like developing long-term relationships with my patients. It’s heartwarming when someone comes back to share about how treatment had a positive impact on their lives. Some are in tears talking about how they felt before compared to how they feel now. That's the driving force behind what we do.

Phillip LoSavio, MD
Board-certified otolaryngologist, Phillip LoSavio, MD, MS, is a sleep surgeon who specializes in treating sleep apnea and related upper airway problems, such as nasal airway obstruction, deviated septum, tonsil enlargement, sinusitis and snoring.
Learn more about Dr. LoSavio
Sleep Surgery at UChicago Medicine
UChicago Medicine's sleep surgery program provides personalized treatment plans using advanced technologies to diagnose and treat sleep apnea, including drug-induced sleep endoscopy, Inspire therapy and surgery to restore your total sleep wellness.
Learn more about sleep surgery