What to know about living liver donation

Each year, there are far more patients on the organ transplant waiting list than there are organ donors. One way to increase the number of possible transplants is through living donation. The liver is one of the few organs that can be transplanted from living donors by using a segment or part of the liver. This can be done safely because of the ability of the liver to regenerate or grow back to full size in both the donor and the recipient.
Who can be a living liver donor?
Adults ages 18 to 55 years old who have normal and healthy liver function are able to be a living liver donor. The living donor must be free from disease and have the right kind of liver anatomy, which is determined by sophisticated imaging. The donor must be a compatible blood type to the recipient.
Read our Tips for Finding an Organ Donor
Why is living donor liver transplant desirable?
In the United States, more than 13,000 people are on the waiting list to receive a liver, but each year approximately 1,500 patients die waiting. A living liver transplant can be scheduled electively before the onset of life-threatening complications while waiting for a liver from a deceased donor. A living donor can assure the recipient receives a healthy portion of the liver with minimal damage as the surgeries happen consecutively. The surgery can also be scheduled when the recipient is in better health and the best chance for a successful transplant.
What is involved in the donor evaluation process?
A potential living liver donor will go through a very detailed evaluation, including blood tests and image studies to check the quality and anatomy of the liver. The process also includes meetings with members of the liver transplant team and other medical services. All of these consultations, tests and procedures will help us decide if the individual is able to become a living liver donor and rule out any medical, surgical, psychological or social barriers that would prevent them from safely being considered as a living donor.
Does the organ donor have to be related to the organ recipient?
Living donors do not have to be related to the recipient. While many people wish to donate a part of their liver to a family member, a person can donate their liver to a friend, coworker or even a stranger.
Are there risks to living donation surgery?
As with any major surgery, liver donation surgery can include complications such as bleeding, infection, heart complications, blood clots and stroke. Donor safety is our main priority, and the multidisciplinary team at UChicago Medicine will evaluate all the potential risks and discuss them with a donor before the procedure. Death is extremely rare but has occurred in a few cases.
How should the living donor prepare for liver transplant surgery?
A living donor liver transplant nurse coordinator is assigned to every donor. The nurse coordinator will help answer any questions or concerns the donor might have regarding the process. All living donors should take basic health measures to ensure surgery goes smoothly and lessen the recipient’s risk of rejecting the liver.
If the donor is a light smoker, they should stop smoking at least one month prior to the liver donation surgery. Smoking can add risks to surgery. Prior to surgery, the donor must refrain from alcohol and drugs. The donor will also need to inform the living donor transplant nurse coordinator of any medications they take. Donors should stop oral contraceptive use at least six weeks prior to living donation to prevent blood clots after surgery. Alternative forms of birth control can be used in the interim, but it is recommended the donor consult with their gynecologist.
How much of the donor’s liver will be removed?
The percentage of the liver that is removed from the donor will depend on their age and size of the patient receiving the transplantation. In general about 50% to 60% of the liver is removed from the donor and transplanted to the recipient.
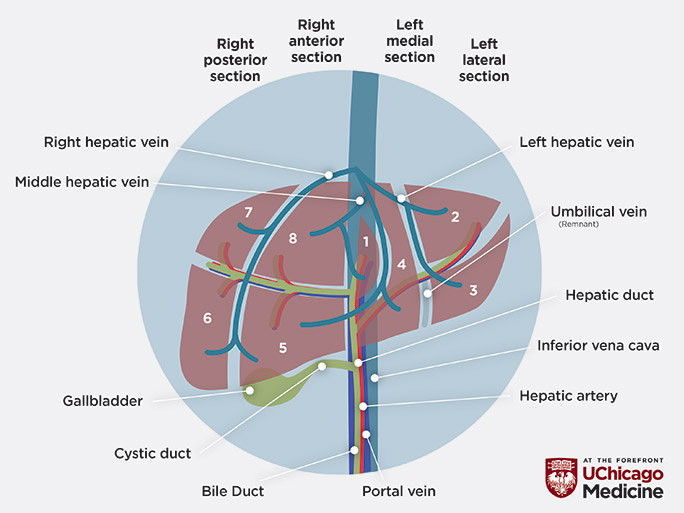
Depending on the surgery, you might donate the left or right lobe. A right lobe donation removes about 60% of the liver; a left lobe donation removes about 40%.
Will the liver grow back?
The partial livers in both the living donor and the recipient will grow to provide normal liver function.
How long will the living liver donor have to stay in the hospital after surgery?
After surgery, the donor will be transferred to a surgical intensive care unit for the first 24 hours to be closely monitored. The following day the donor will be transferred to the transplant floor for five to seven days before returning home.
How long will the liver recipient have to stay in the hospital after surgery?
Following surgery, the liver transplant patient will be transferred to the surgical intensive care unit for the first 24 to 48 hours and be closely monitored. After that period, the patient will be transferred to the transplant floor and could remain there for two to five days before returning home.
Will insurance cover the cost of a liver transplant?
All medical costs related to the donation are covered by the recipient’s insurance.
Are there any assistance programs for living liver donors?
The National Living Donor Assistance Center is a nationwide system that provides reimbursement of travel, lodging and food expenses to individuals being evaluated for and/or undergoing living organ donation. Priority is given to those who could not otherwise afford to donate.
